If you're reading this, chances are you've lost a tooth — or you've been told you're about to lose one. Maybe it happened because of decay, an accident, or gum disease that progressed quietly over the years. Whatever brought you here, we want you to know something upfront: you're not alone, and you have good options.
About 120 million Americans are missing at least one tooth, and more than 36 million have lost all of their natural teeth. Dental implants have become one of the most trusted ways to replace what's been lost — not just the tooth itself, but the confidence and comfort that come with it. But implants are a significant decision, both financially and medically, so it's worth understanding exactly what you're getting into before you commit.
This guide walks you through how dental implants work, what the procedure actually involves, what they cost, what the risks are, and how to know if they're right for you. No sales pitch — just the information you need to make a decision that feels right.
What Exactly Is a Dental Implant?
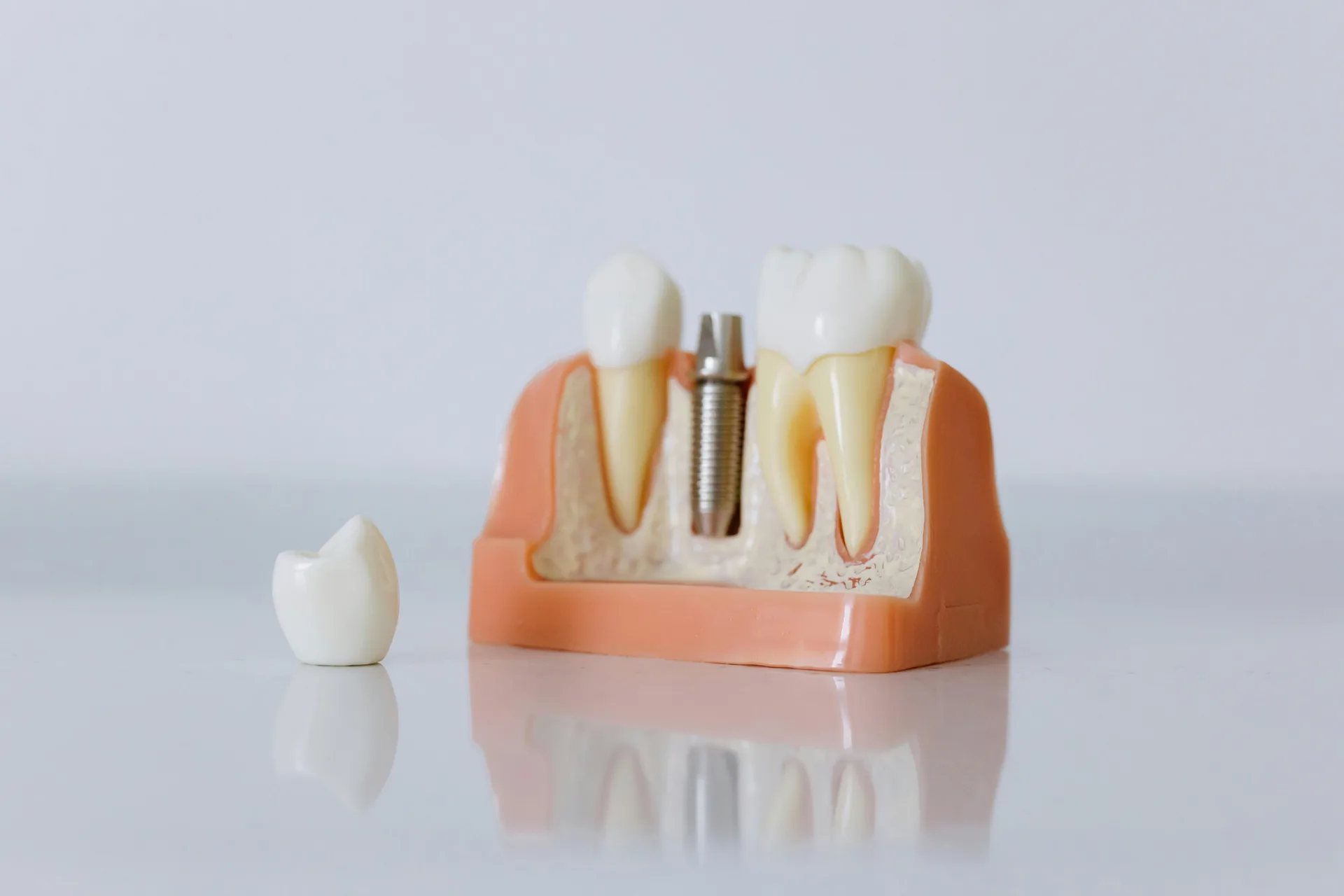
A dental implant is a three-part system designed to replace a missing tooth from root to crown. Unlike dentures or bridges that sit on top of your gums or attach to neighboring teeth, an implant is anchored directly into your jawbone — which is why it feels and functions so much like a natural tooth.
Here's how the three parts work together:
The abutment — a small connector piece that sits on top of the implant post, just above the gumline. It links the implant to the visible tooth.
The crown — the custom-made, tooth-colored piece that attaches to the abutment. This is the part you see when you smile.
The U.S. Food and Drug Administration (FDA) regulates dental implant systems and requires manufacturers to demonstrate safety and effectiveness before they can be marketed. The materials — primarily titanium — are biocompatible, meaning they're designed to work with your body without causing allergic reactions. True titanium allergies are extremely rare.
Are You a Good Candidate?
Most healthy adults with one or more missing teeth are good candidates for dental implants. But "most" doesn't mean "everyone," and it's important to have an honest conversation with your dentist before moving forward.
Generally, you're a good candidate if you have adequate jawbone density to support the implant (or are willing to undergo bone grafting), your gums are healthy, you don't smoke or are willing to quit before and during healing, and you don't have uncontrolled chronic conditions that could impair healing.
When implants may not be the right fit
Certain conditions can make implants riskier or less likely to succeed. This isn't meant to discourage you — just to give you an honest picture:
Active gum disease — untreated periodontal disease can compromise the bone and soft tissue that implants depend on. This usually needs to be treated first.
Smoking — nicotine constricts blood vessels and reduces oxygen supply to the gums and jawbone, delaying healing and increasing infection risk. Most dentists will strongly recommend quitting before proceeding.
Recent radiation therapy to the head or neck — radiation can compromise bone quality and healing capacity. Your oncologist and dental surgeon will need to work together on timing.
Certain medications — immunosuppressants, blood thinners, and some osteoporosis drugs can affect healing or bone quality. Always share your full medication list with your dentist.
If you've been told in the past that you're "not a candidate," it may be worth getting a second opinion. Advances in bone grafting, mini implants, and guided surgical techniques have expanded eligibility significantly over the past few years.
What the Procedure Actually Looks Like
One of the biggest sources of anxiety around implants is not knowing what to expect. So here's a straightforward breakdown of the process, start to finish. Keep in mind that your timeline may vary depending on whether you need any prep work like extractions or bone grafting.
The entire process, from consultation to final crown, typically spans 4 to 9 months. Some practices now offer "same-day" or "teeth-in-a-day" protocols where a temporary crown is placed immediately after implant surgery — but this depends on your bone quality and isn't appropriate for every case.
Recovery: What Does It Actually Feel Like?
Let's be honest about this, because it's the question most people are afraid to ask. After the implant is placed, you can expect some swelling, mild bruising, and soreness for the first few days. Most patients manage this with over-the-counter pain relievers. The discomfort is real, but it's temporary — and most people say it was less painful than they expected.
For the first week or two, you'll want to stick to soft foods and avoid the surgical area when chewing. Your dentist will give you specific care instructions, which typically include gentle rinsing and avoiding straws or smoking. If pain or swelling worsens after the first week rather than improving, contact your dentist — it could indicate an infection or other complication that needs attention.
Risks and Complications: An Honest Look
No medical procedure is without risk, and dental implants are no exception. The good news is that serious complications are uncommon. But you deserve to know what they are before you make this decision.
Infection at the implant site is the most commonly cited risk. Maintaining good oral hygiene and following your dentist's post-op instructions significantly reduces this risk. Nerve damage, while rare, can occur if the implant is placed too close to a nerve — causing numbness, tingling, or pain in the lips, chin, or gums. This is one reason why 3D imaging and computer-guided placement have become so valuable.
Implant failure — where the bone doesn't properly fuse with the implant — happens in a small percentage of cases. Clinical data suggests success rates of 95–98% within the first 5 to 10 years. The U.S. has a reported failure rate of about 6%, which factors in all types of cases, including higher-risk patients. If an implant does fail, it can usually be removed and re-attempted after healing, with a roughly 90% success rate on the second attempt.
Peri-implantitis is a condition similar to gum disease that affects the tissue around an implant. It can develop years after placement — particularly in patients who smoke, have a history of gum disease, or don't keep up with regular dental hygiene. This is why long-term maintenance matters just as much as the surgery itself.
What Do Dental Implants Cost?
Cost is often the biggest barrier — and unfortunately, there's no single number that applies to everyone. The total depends on where you live, the complexity of your case, whether you need bone grafting or extractions, and the materials used.
That said, here are the general ranges as of 2026:
| Procedure | Typical U.S. Cost Range |
|---|---|
| Single implant (post + abutment + crown) | $3,000 – $6,000 |
| Bone grafting (if needed) | $500 – $3,000 |
| Multiple implants with bridge | $3,250 – $30,000 |
| Full arch replacement (one jaw) | $15,000 – $30,000 |
| Full-mouth restoration (both jaws) | $25,000 – $60,000+ |
Dental insurance coverage for implants varies widely. Some plans cover the crown portion but not the surgical placement. Others may categorize implants as "major" work with 50% coverage up to an annual maximum (typically around $1,500). If your plan doesn't cover implants, ask about third-party financing options like CareCredit, in-office payment plans, or using a Health Savings Account (HSA) or Flexible Spending Account (FSA).
One important perspective on cost: implants are more expensive upfront than bridges or dentures, but they're designed to last decades — potentially a lifetime with proper care. Dentures and bridges typically need replacement every 5 to 15 years, and those repeat costs add up. For many patients, implants turn out to be the more economical choice over the long run.
Implants vs. Bridges vs. Dentures
Implants aren't the only option for replacing missing teeth, and they're not always the best option for every situation. Here's a fair comparison:
| Factor | Implants | Bridges | Dentures |
|---|---|---|---|
| Lifespan | 15–25+ years | 5–15 years | 5–10 years |
| Bone preservation | Yes — stimulates jawbone | No | No |
| Affects adjacent teeth | No | Yes — requires filing down neighbors | No |
| Look and feel | Most natural | Natural appearance | Can feel bulky; may shift |
| Upfront cost | Highest | Moderate | Lowest |
| Maintenance | Brush, floss, regular checkups | Brush, floss carefully around bridge | Daily removal, cleaning, adhesive |
There's no shame in choosing any of these options — they all serve a purpose. What matters is that you understand the trade-offs and choose what aligns with your health, your budget, and your lifestyle. A good dentist will walk you through all three honestly, not push you toward the most expensive one.
Questions to Ask Your Dentist Before Moving Forward
When you're sitting in that consultation chair, it can be hard to think of everything you want to ask. Here are the questions we'd suggest bringing with you:
About the procedure: How many implants have you placed, and what's your success rate? What type of implant material will you use, and why? Will the surgery be guided by 3D imaging?
About cost: What's the full cost breakdown — implant, abutment, crown, and any prep work? Does my insurance cover any portion? Do you offer payment plans or financing?
About recovery: What should I expect for pain and downtime? What are the signs of a complication I should watch for? When can I return to normal eating?
A dentist who takes time to answer these questions thoroughly — without rushing you or making you feel pressured — is one worth trusting with this decision.
Final Thoughts
Losing a tooth can feel like more than just a dental problem. It can affect how you eat, how you speak, how you smile in photos, and how you feel about yourself in everyday conversations. If that resonates with you, please know that those feelings are completely valid.
Dental implants aren't a miracle — they're a well-researched, well-proven medical procedure with real benefits and real limitations. The best outcomes happen when patients go in informed, choose their provider carefully, and commit to the aftercare. If you're considering implants, take the time to get a proper consultation, ask the hard questions, and don't rush the decision. Your oral health is worth the effort.
Looking for a Trusted Implant Dentist?
Browse our curated listings to find experienced, highly rated dental implant providers in your city.
Sources & References
- U.S. Food and Drug Administration — Dental Implants: What You Should Know
- American Dental Association — How to Find a Dentist (MouthHealthy.org)
- PMC — Risks and Complications Associated with Dental Implant Failure: Critical Update
- PMC — The Future of Dental Implants: Trends, Technologies, and Patient Considerations (2025)
- Medical News Today — Dental Implants Problems: Complications, Symptoms, Risks
- WebMD — Risks Associated With Dental Implants
- Healthline — Are Dental Implants Safe? Potential Risks
- MetLife — How Much Do Dental Implants Cost?
- GoodRx — How Much Do Dental Implants Cost?
- Dental Implant Statistics in the U.S.: Dentistry Report 2026