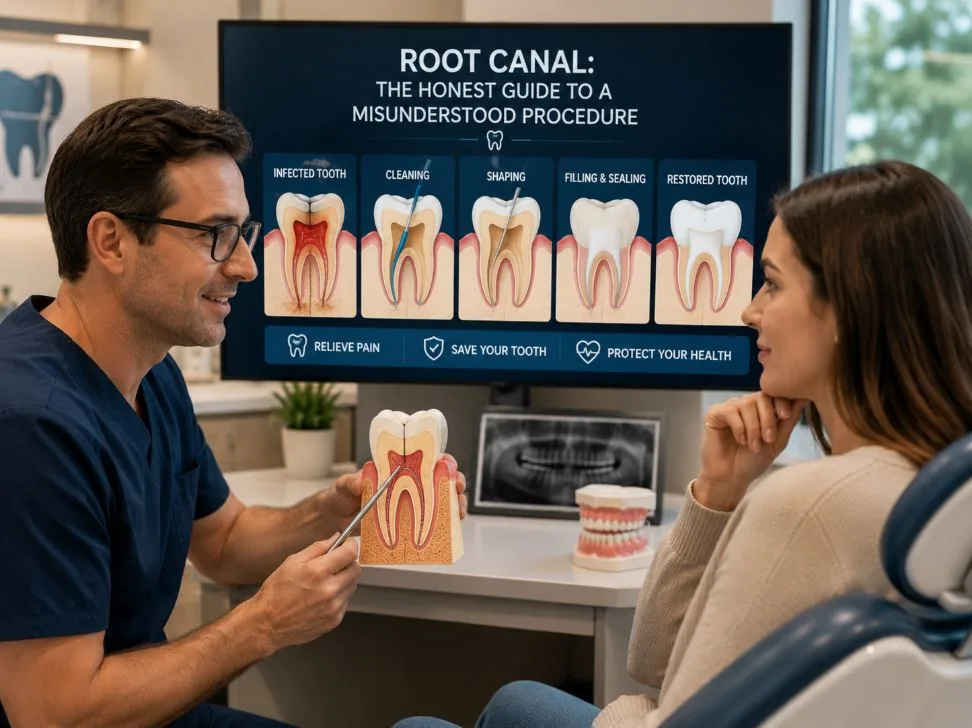
No dental procedure is more misunderstood than the root canal. The cultural shorthand — "I'd rather have a root canal than do that" — survives because the procedure used to be associated with significant pain, the literature on it is dense, and a small but loud strand of pseudoscience continues to claim that root canals cause cancer and chronic disease. None of that reflects the actual modern procedure, the actual peer-reviewed evidence, or the position of mainstream dentistry. Modern endodontic treatment is largely painless, supported by a century of clinical research, and one of the most successful tooth-preserving interventions available.
This guide walks you through what a root canal actually is and why teeth need them, what the procedure honestly feels like, the science vs. the myths, the real success rates from peer-reviewed long-term studies, what it costs in 2026, when retreatment or surgery makes sense after a failed root canal, and how to choose between an endodontist and a general dentist. Sources for every clinical claim are listed at the bottom — primary peer-reviewed literature, American Association of Endodontists position papers, ADA Council on Scientific Affairs statements, and Cochrane systematic reviews. Nothing here is editorial speculation; if you don't trust any specific claim, the source is one click away.
One thing worth saying up front: the goal of this post is to give you the information your dentist's chair-side conversation rarely has time for. Root canal decisions involve real tradeoffs — between saving a tooth and replacing it, between general-dentist treatment and specialist referral, between immediate relief and longer-term outcome. You deserve to make that decision with the actual facts in front of you.
What a Root Canal Actually Is
Inside every tooth is a small chamber containing soft tissue — pulp — made up of nerves, blood vessels, and connective tissue. The pulp runs from the center of the crown down through narrow channels (root canals) to the tip of each root. When that pulp becomes infected — typically because deep decay has reached it, or because trauma has disrupted its blood supply, or because a crack has opened a pathway for bacteria — the tooth has two paths forward: extract it, or treat the infection by removing the pulp, cleaning and disinfecting the canal system, and sealing the space.
The second path is what dentists call endodontic treatment — what patients usually call a "root canal." The procedure preserves the tooth's external structure (the part you chew with) by removing the source of infection inside it. Most root-canaled teeth, properly restored with a crown afterward, function for decades.
Root canal treatment is one of nine specialties recognized by the American Dental Association. The specialist is called an endodontist — a dentist who completed dental school and then a 2- to 3-year accredited endodontic residency focused exclusively on diagnosing and treating diseases of the dental pulp and periapical tissues. General dentists also perform root canals, particularly on simpler cases (single-canal anterior teeth, straightforward premolars), but endodontists handle the complex cases (curved roots, calcified canals, retreatments, surgical apicoectomies) that exceed routine general-dentistry scope.
What the Procedure Actually Looks Like
Modern root canal treatment is highly procedurally standardized. Whether your case takes one or two visits depends on the complexity and the dentist's preference, but the steps are consistent.
Total chair time for a routine single-tooth root canal is typically 60-90 minutes for a single-canal anterior tooth, and 90-120 minutes for a multi-canal molar. Two-visit cases add a 1-2 week interval between visits when the canal needs additional disinfection time before obturation.
What It Actually Feels Like
This is the question patients are most afraid to ask, and the answer is the most reassuring part of the whole procedure. The reputation of root canals as exceptionally painful is rooted in the procedure as it was performed 40-50 years ago — without microscopes, without modern rotary instrumentation, without nickel-titanium files, and often without adequate anesthesia for inflamed pulp. The procedure performed in 2026 by a competent endodontist or general dentist is fundamentally different.
Multiple peer-reviewed studies measuring intra-procedural pain on Visual Analog Scale (VAS) ratings have found that pain scores during modern endodontic treatment are statistically equivalent to or lower than pain scores during routine fillings — once adequate anesthesia is established. The American Association of Endodontists publishes patient-survey data showing the majority of patients describe the experience as no more uncomfortable than a filling.
What you'll actually experience: about 15 seconds of pinch from the anesthetic injection, a few minutes of pressure as the dentist confirms numbness, then 60-120 minutes of mild pressure sensations and the sound of instruments. Post-operative discomfort for 24-48 hours afterward is normal — typically managed with over-the-counter ibuprofen, sometimes briefly with a stronger prescription. Severe post-op pain is uncommon and usually signals a complication that should be addressed promptly.
The pain people associate with "root canals" is actually almost always the pain of the infection that led them to need a root canal in the first place. The procedure resolves that pain. By 24-48 hours after treatment, most patients report substantially less discomfort than before they walked into the office.
Endodontist or General Dentist?
Both can perform root canals legally. The decision should depend on case complexity, your dentist's experience with similar cases, and the specific anatomy of the tooth being treated.
| Best fit for general dentist | Best fit for endodontist |
|---|---|
| Single-canal anterior teeth | Multi-canal molars (especially upper second molars) |
| Straightforward premolars | Curved or calcified canals |
| Routine cases without complicating anatomy | Retreatment of previously failed root canals |
| Patients without significant medical complexity | Surgical cases (apicoectomy) |
| Cases your dentist specifically does well | Trauma cases, immature roots, special-needs sedation |
Long-term outcome studies consistently show small but measurable advantages for endodontist-treated cases on complex teeth — primarily because endodontists operate exclusively under microscopes, use specialty-tier instrumentation, and see complex cases in volume. For straightforward single-canal cases, outcomes are similar. The American Association of Endodontists maintains a public referral directory and a board-certification verification tool through the American Board of Endodontics.
How Successful Are Root Canals, Honestly?
Long-term success rates depend on the tooth, the case complexity, and the operator. Cochrane Reviews and multi-decade outcome studies in the Journal of Endodontics consistently report that initial endodontic treatment achieves long-term success in 86-98% of cases when the work is done to current standards and the tooth is properly restored afterward.
"Success" in these studies is defined rigorously — clinical absence of symptoms and radiographic evidence of healing of any periapical lesion at multi-year follow-up. The number is not "the tooth still feels okay"; it's the actual evidence-based outcome.
| Scenario | Long-term success rate (peer-reviewed) |
|---|---|
| Initial root canal, vital pulp, no periapical lesion | ~95-98% at 5-10 years |
| Initial root canal, infected pulp, no apical lesion | ~90-95% |
| Initial root canal with periapical lesion present | ~80-90% |
| Endodontic retreatment (failed prior root canal) | ~70-85% |
| Surgical apicoectomy after failed retreatment | ~75-90% |
Two factors significantly affect the numbers: quality of the coronal restoration after the root canal (a properly placed crown roughly doubles the long-term success vs. a poorly fitting temporary that leaks), and operator skill and equipment (cases done with rubber dam, microscope, and 3D imaging substantially outperform cases done without). Both factors are within your control when you choose your provider.
The Myths: What the Pseudoscience Actually Claims, and What the Evidence Says
The "root canals cause cancer" / "root canals cause chronic disease" claims that circulate online trace back to a single 1920s researcher — Weston Price — whose focal infection theory proposed that infections in the mouth could spread systemically and cause disease elsewhere in the body. Price's experiments did not meet modern scientific standards, were not replicable, and were definitively rejected by the dental research community by the 1950s. The American Dental Association and the American Association of Endodontists have published explicit position papers refuting the focal infection theory and the claim that endodontically treated teeth pose any unusual systemic risk.
The pseudoscientific claim continues to circulate primarily through alternative-medicine practitioners and a few high-profile online personalities who repackage Weston Price's century-old, methodologically discredited research as "the truth they don't want you to know." It isn't. The evidence base is large, consistent, and publicly verifiable.
If you've encountered the "Root Canal Cover-Up" claim and want to evaluate it on the merits, the right path is to read the AAE position paper, the underlying cohort studies, and the systematic reviews — sources linked at the bottom of this post — and compare them with the claims of the alternative-medicine sources making the original assertions. The asymmetry between the two will be obvious within the first paragraph.
When a Root Canal Fails: Your Options
Roughly 5-15% of root canals will eventually fail, depending on case complexity, restoration quality, and time horizon. When that happens — confirmed by symptoms, X-ray evidence of new or persisting infection, or a tooth that becomes painful again months or years later — you have three primary options. Each has different success rates, costs, and tradeoffs. Choosing among them is one of the more confusing decisions in dentistry, but the framework is actually fairly clear once you understand it.
The decision between retreatment, apicoectomy, and extraction is case-specific and benefits from a second-opinion consultation with an endodontist who can evaluate the imaging and the specific failure mode. Don't accept a same-day extraction recommendation on a previously treated tooth without first consulting an endodontist about whether retreatment or surgery is viable — once the tooth is gone, your options narrow permanently.
What a Root Canal Actually Costs in 2026
Cost varies by tooth (anterior teeth are simpler than molars), provider (endodontists charge specialty rates that are typically 20-40% higher than general dentists), and geography. Here are the realistic U.S. ranges:
| Tooth Type | General Dentist | Endodontist (Specialist) |
|---|---|---|
| Anterior (front) tooth | $700 – $1,300 | $900 – $1,600 |
| Premolar (bicuspid) | $800 – $1,500 | $1,100 – $1,900 |
| Molar (back tooth) | $1,200 – $2,000 | $1,400 – $2,400 |
| Endodontic retreatment | $1,000 – $1,800 | $1,400 – $2,800 |
| Apicoectomy (per root) | — | $1,000 – $2,500 |
| CBCT (3D scan) | $200 – $400 | $200 – $400 |
| Crown (after root canal) | $1,000 – $2,500 | — |
The crown is a separate cost and is essential for posterior teeth — leaving a root-canaled molar without a crown roughly halves the long-term success rate. Budget for both. Most dental insurance plans cover endodontic treatment as a "major" procedure at 50-80% up to the annual maximum (typically $1,500-2,000), with similar coverage for the post-treatment crown.
Five Questions to Ask Before Treatment
Red Flags That Should Stop You
No rubber dam isolation — non-negotiable per AAE standards. A practice not using rubber dam isolation is working below the standard of care.
Same-day root canal recommendation without imaging — endodontic treatment requires an X-ray at minimum and often a CBCT. A walk-in same-day treatment plan without proper imaging is rushing the diagnostic phase.
Pressure to commit before consulting an endodontist on a complex case — particularly retreatments or curved-canal molars. A confident general dentist will refer the case if it exceeds their skill set; one who pressures you to stay in-practice on a complex case is being protective of revenue, not patient outcome.
"Root canals always fail" / "Just extract and get an implant" framing — this is sales language disguised as clinical advice. Modern root canals have 86-98% long-term success rates. Implants have ~95% 10-year survival rates. Neither is "always" anything. The right answer depends on your specific case, not on the practice's preferred procedure mix.
How Smyleee Helps You Find the Right Provider
Smyleee maintains city-level Top 10 root canal rankings for major U.S. metros, vetting providers on credential signals (residency training, ABE certification, AAE membership), case-volume markers, and aggregate patient feedback rather than raw review counts. Each entry flags whether the practice uses microscopes and CBCT routinely.
Useful starting points if you want a curated shortlist:
- Top 10 Root Canal Specialists in Brooklyn
- Top 10 Root Canal Specialists in San Diego
- Top 10 Root Canal Specialists in Los Angeles
- Top 10 Root Canal Specialists in Miami
- Top 10 Root Canal Specialists in Charlotte
For specific situations, dedicated guides cover what root canal pain actually feels like, what to do when a root canal fails, choosing between apicoectomy and retreatment, the science behind root canal safety, and when to save the tooth vs. replace it.
Final Thoughts
Root canal treatment is the most-misunderstood mainstream dental procedure. The reality is closer to the opposite of the reputation: it's a high-success, evidence-supported, technically standardized procedure that preserves natural tooth structure for decades when done well. The pain reputation reflects the procedure as it was a half-century ago, not the procedure as it's practiced now. The "danger" reputation reflects a 1920s pseudoscientific theory that the dental research community discarded by the 1950s and that mainstream science has continued to refute ever since.
What separates good outcomes from regretted ones is almost never whether the procedure was a root canal vs. something else — it's whether the right provider used the right technique on the right case. Endodontist for complex cases. Microscope and rubber dam always. CBCT for difficult anatomy. Proper restoration afterward. Honest second opinion when something doesn't add up.
Take the time. Ask the questions. Get the imaging. Don't accept the framings that have nothing to do with the actual evidence. The tooth you keep today is the one you don't have to replace tomorrow.
Find a Vetted Root Canal Specialist
Browse Smyleee's curated, credential-vetted directory of endodontists and general dentists experienced in root canal treatment — with microscope-use flags, ABE certification markers, and aggregate patient ratings.
Sources & References
- American Association of Endodontists — Position Statements (Endodontic Treatment Is Safe; Cracked Teeth; Treatment Standards)
- American Association of Endodontists — Clinical Resources Library & Treatment Standards
- American Board of Endodontics — Board Certification Standards & Specialist Verification
- American Dental Association — Endodontics Oral Health Topic & Council on Scientific Affairs Statement
- Cochrane Reviews — Endodontic Treatment Outcome Systematic Reviews
- Journal of Endodontics — Peer-Reviewed Research on Treatment Outcomes & Pain
- AAE — Endodontic Treatment Is Safe (Patient Resource & Position Paper)
- PubMed / NCBI — Primary Literature Search on Endodontic Outcomes & Focal Infection Theory
- U.S. Food and Drug Administration — Dental Device & Material Safety Guidance
- Centers for Disease Control and Prevention — Oral Health & Infection Control Resources
- MetLife Oral Fitness Library — Root Canal Cost Reference
- GoodRx — Root Canal Cost Guide
- CareCredit — Root Canal Treatment Financing
- American Dental Association MouthHealthy — Patient Guide to Root Canals
- IRS Publication 502 — Medical and Dental Expenses (HSA / FSA Eligibility)